In 2019, around 16.5% of the American population was aged 65 years or older; by 2050, this figure is projected to increase to 22% [1]. One prevalent issue associated with aging that significantly impacts the elderly is edentulism, which refers to the condition of having missing teeth. The ratio of individuals with edentulism to those with natural teeth is approximately 2:1. Currently, about 23 million people are completely edentulous, while an additional 12 million are missing teeth in one arch. Notably, 90% of edentulous individuals wear dentures, which can be categorized as either fixed or removable [2]. A fixed denture consists of prosthetic teeth that are securely anchored to artificial gum tissue positioned above the natural gum line [3]. Removable dentures can be classified into complete and partial types. The latter typically includes a cast metal framework, acrylic clasps, and flexible components, all molded to resemble the natural gums. Complete dentures serve as full-arch prosthetics, replacing all missing teeth in a particular arch [3-4].
For the elderly, dentures offer both functional and cosmetic advantages, enhancing their ability to eat, speak, and smile with confidence. However, the use of dentures is not without risks. Issues such as ill-fitting dentures, improper usage, and inadequate oral hygiene can lead to complications like gum irritation, ulcerations, and a condition known as denture stomatitis [5]. Furthermore, the surfaces of dentures can serve as breeding grounds for various pathogens, contributing to serious health concerns like aspiration pneumonia, bad breath (halitosis), and potentially life-threatening infections such as infective endocarditis and septic meningitis due to biofilm accumulation. Additionally, the elderly are at higher risk for accidental aspiration or ingestion of dentures, particularly those with conditions like alcohol dependence, advanced dementia, stroke, or epilepsy [6]. The consequences of ingesting dentures can be dire, including necrosis, perforation, internal bleeding, and obstruction [6-7].
These clinical challenges and severe health risks can often be mitigated through proper guidance from healthcare providers, which may include primary care physicians, dentists, and dental hygienists. Despite the necessity for greater education on this topic, there is a concerning lack of accessible, evidence-based information regarding effective cleaning practices for dentures and their proper usage [8]. Research indicates that at least 40% of elderly denture users do not engage in proper disinfection practices or fail to remove their dentures at night, resulting in a twofold increase in serious pneumonia cases among this demographic [9]. Therefore, obtaining professional advice on the appropriate use and maintenance of dentures is crucial, particularly for elderly patients and their caregivers [8].
The insufficient education surrounding denture care, combined with the limited availability of routine dental services for underserved and aging populations, exacerbates the issues at hand [9]. Many older adults struggle to afford the preventive and rehabilitative care they need [9]. Enhancing the oral health literacy of patients is also essential in preventing future complications [8].
To address these concerns, we conducted a systematic review aimed at evaluating the complications, infections, and potentially life-threatening conditions associated with inadequate denture usage and poor oral hygiene in the geriatric population utilizing removable dentures. Our research also investigated factors contributing to declining oral health among the elderly, particularly focusing on conditions such as diabetes, substance abuse, and tobacco use [10-11]. The ultimate goal of this review is to promote effective, dentist-recommended, evidence-based guidelines for denture care and optimal usage.
Comprehensive Methodology for Assessing Denture-Related Complications
This systematic review was structured and its findings were reported in adherence to the Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) 2020 Guidelines [12].
Robust Search Strategy for Relevant Literature
A comprehensive computer-aided search was conducted across several medical databases, including PubMed, PubMed Central (PMC), MEDLINE, and Cochrane Library, spanning from December 14, 2021, to January 14, 2022. This search utilized a variety of keyword combinations, such as “Dentures and complications,” “Dentures and halitosis,” “Dentures and pneumonia,” “Dentures and stomatitis,” “Dentures and ulcerations,” “Dentures and infections,” and “Dentures and oral hygiene.” Additionally, we employed a MeSH (Medical Subject Headings) search strategy to enhance the precision of our search results: (“Denture, Partial, Removable/adverse effects”[Mesh] OR “Denture, Partial, Removable/classification”[Mesh] OR
“Denture, Partial, Removable/etiology”[Mesh] OR “Denture, Partial, Removable/microbiology”[Mesh] OR
“Denture, Partial, Removable/pharmacology”[Mesh] OR “Denture, Partial, Removable/psychology”[Mesh] OR
“Denture, Partial, Removable/virology”[Mesh]). We also utilized the search term “Dentures and infections or complications or ulcerations or stomatitis or pneumonia or halitosis or oral hygiene” within the Cochrane Library. The search results are detailed in Tables 1–2.
Defined Inclusion and Exclusion Criteria for Article Selection
We meticulously selected articles published between 2012 and 2022, which were written in English, involved patients aged 65 years or older, and were globally published. Only studies involving human participants were included in our review. Articles were excluded if they required purchase for access, if they were categorized as gray literature, if they did not directly relate to our research objectives, or if only abstracts were available for review.
Thorough Selection Process for Relevant Studies
All articles identified through our search strategy were imported into the Endnote application, where duplicates were removed. Each article was screened based on title and abstract by the first and second authors, AD and ZN, who independently assessed the relevance. Any discrepancies regarding article eligibility were resolved through discussion, applying the established inclusion and exclusion criteria before reaching a consensus. The remaining articles underwent a detailed full-text review to filter out any that were not relevant.
Systematic Data Collection Process for Quality Evaluation
Upon finalizing the articles for our systematic review, all authors participated equally in evaluating each study for quality assurance and extracting the necessary information to be included in our comprehensive review article.
Comprehensive Quality Assessment of the Selected Studies
We critically appraised randomized clinical trials using the Cochrane Risk of Bias Assessment Tool 2 [13], while systematic reviews were evaluated using the Assessment of Multiple Systematic Review (AMSTAR) tool [14]. Additionally, the Joanna Briggs Institute (JBI) critical appraisal checklist was applied for case reports [15], and the Newcastle Ottawa Quality Assessment tool was utilized for observational studies [16]. Lastly, the Scale for the Assessment of Narrative Review (SANRA) was employed for publications lacking specific methodologies [17]. Only studies with a quality appraisal score exceeding 60% were included in the systematic review.
Results of Our Comprehensive Review
Identification and Selection of Relevant Studies
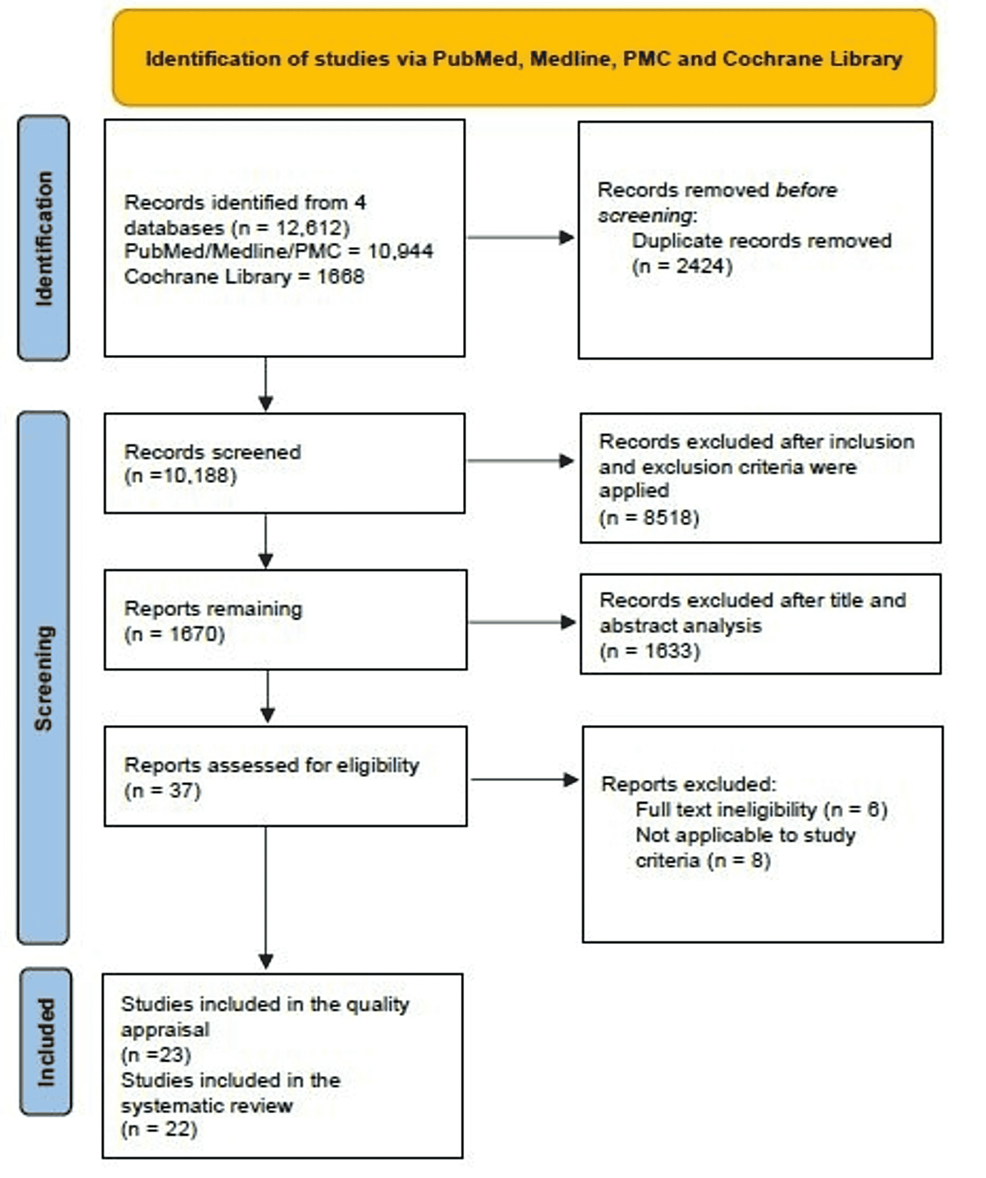
Through our exhaustive search, we initially obtained 12,612 articles that met the established search criteria. This included 10,944 publications sourced from PubMed, PMC, and Medline, alongside 1,668 articles from the Cochrane Library. The Endnote application facilitated the removal of duplicate articles, resulting in 10,188 remaining articles after eliminating 2,424 duplicates. Applying our inclusion and exclusion criteria led to the exclusion of 8,518 articles. Consequently, 1,670 articles were selected for further evaluation through title, abstract, and full-text analysis. Ultimately, 37 articles remained after the title and abstract analysis; six were excluded following the full-text review. An additional eight publications were excluded for various reasons or because they did not meet the study criteria. Thus, out of the remaining 23 articles, we conducted a quality assessment on five case reports, 11 observational studies (three cross-sectional studies, two case-control studies, four prospective cohort studies, and two retrospective cohort studies).
We also reviewed three systematic reviews, three randomized control trials (RCTs), and one narrative review. Following quality appraisal, one RCT was excluded due to a low score, resulting in 22 publications being included in our study. A complete Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flow diagram is presented below in Figure 1 [12]. Table 3 lists all publications included in this systematic review, while Tables 4–8 display the quality assessments of all review articles incorporated in this systematic review.
<div class="article-attachment-wrap table-attachment-wrap" data-number="4" id="table-anchor