A warning to readers, some images and details of this story may be disturbing.
“Cherish every moment with loved ones suffering from dementia, as each moment is invaluable.”
– Jason Keller
A pair of siblings, Santaya Garnot and Jason Keller, are bravely voicing their concerns regarding the Simon Fraser Lodge in Prince George. They allege that the negligent care provided by the facility significantly contributed to the tragic death of their mother, Kelly Ashton. After suffering multiple falls within a single day, the family believes that the lack of adequate supervision and care protocols directly led to her demise.
Following their mother’s passing, Garnot and Keller took it upon themselves to investigate further. They sought access to the Lodge’s incident reports, internal investigation summaries, and hospital records related to their mother’s falls through Northern Health. This was an essential step in understanding the circumstances surrounding Kelly’s care and the events leading up to her decline.
Ashton, a 62-year-old patient diagnosed with dementia, had been residing at Simon Fraser Lodge since mid-2020. Her condition was characterized by a progressive decline in cognitive functions, impacting her memory, communication, and physical stability. The Public Health Agency of Canada defines dementia as an umbrella term covering various symptoms that impair brain function, emphasizing its chronic nature and the subsequent challenges it poses for both patients and caregivers.
“Mom was in the late stages of dementia,” Keller explained. “Even though her condition had advanced, she could still express basic sentiments like ‘I love you.’ She maintained her ability to eat, walk, and engage in conversation, which made our time together special and meaningful.”
According to the records obtained by the family, during a single day in November, Ashton experienced two falls—a concerning and frequent occurrence for dementia patients. Alarmingly, she was only transported to the hospital after her family intervened. This raises serious questions about the care protocols in place at the Lodge and whether they were adequately followed.
Hospital records obtained by the family confirmed that Ashton had sustained multiple fractures in her neck due to these falls. Tragically, she passed away less than a month later, highlighting the severe consequences that can arise from inadequate care.
On the morning of November 9th, 2022, Garnot and Keller received a distressing call from Simon Fraser Lodge informing them that their mother had slipped and fallen, resulting in a head injury. The Lodge maintained an incident report log, which was filled out as events unfolded, followed by a summary generated later on. This documentation, although intended for clarity, contained inconsistencies regarding the details of the incidents.
Both the incident report and the investigation summary indicated that around 12:30 p.m., staff reported flooding from a nearby bathroom that had encroached into Ashton’s bedroom. The investigation summary records noted, “Night staff observed the resident sitting at the edge of her bed, displaying signs of physical aggression.” Furthermore, staff documented that she required assistance with her soiled clothing.
According to the incident report, staff members managed to change her at 2:36 a.m. and administered medication for “severe agitation” since she was reportedly verbally and physically aggressive during this process. Alarmingly, it was noted that she refused to return to bed and began wandering the halls of the facility independently.
At 4:00 a.m., staff found her on her knees in the living room, exhibiting a bump and cut on her forehead, with blood on the floor.
Despite her ongoing aggression, the incident report documented that she was taken back to her room in a wheelchair, where she was bandaged, assessed, and eventually returned to bed, where she fell asleep. There is a conflicting account between the incident report and the investigation summary regarding the timeline of events and the cleanup of the flooded area.
The investigation summary stated that the flooded water was addressed between 12:50 a.m. and 3:05 a.m.; however, the incident report logged at 9:00 a.m. indicated that care staff had to wake her up to clean the room at 4:00 a.m. Since then, the report noted that the resident had been agitated and drowsy, posing a potential risk for another fall.
Later that same day, after a series of troubling developments, the family was informed that their mother had fallen again and hit her head once more. “My sister was worried,” Keller recalled. “Although Ashton seemed fine initially, she was heavily medicated and appeared to be bumping into walls while walking.”
“My sister expressed her concerns, warning that without close supervision, she could easily fall again. The staff assured her that everything was under control and that they would be closely monitoring her. Yet, shortly after, they called to inform us that she had fallen again,” Keller lamented.
“I visited her later that day,” Garnot recounted. “I insisted that a doctor be called to evaluate her condition, as I was deeply concerned about her level of consciousness and confusion.”
“They reassured me that the doctor had been notified and that she was stable, advising us not to pursue further medical attention.” However, just two hours after my visit, they called again to report another fall,” she said.
The second fall was formally recorded in the incident report logs at 6:20 p.m. on November 9th.
The investigation summary revealed that a dietary staff member witnessed Ashton trip over a wet floor sign that had been carelessly left propped against a wall in a cluttered hallway. Keller criticized this negligence, stating, “The dementia ward is chaotic. Residents are often heavily medicated and have mobility challenges, yet they are expected to navigate around obstacles like that. It makes no sense.”
The incident report described Ashton as being found “screaming” in the hallway, prompting staff to check her vitals and provide an ice pack for her head. A subsequent log entry at 11:50 p.m. noted that she had a bump on her forehead and felt warm to the touch, but staff reported that she appeared comfortable.
“I inquired again, ‘Should I take her to the hospital?’ and their response was, ‘No, she is fine… she has no new injuries, and we will continue to monitor her.’ They assured me that the doctor was informed and deemed her condition acceptable,” Garnot stated.
According to hospital records, the falls led to fractures in her Cervical 1 and Cervical 2 vertebrae, the first two cervical vertebrae of the spine. This alarming injury highlights the critical need for vigilant care and preventive strategies in facilities catering to vulnerable populations.
“The following morning, we requested a care meeting,” Keller shared. During this meeting, they discussed the series of falls with the General Manager and Head Care Nurse of the Lodge.
Keller voiced his concern, saying, “You are fortunate that nothing worse occurred, or we would be having a very different conversation today.”
During the meeting, Ashton was sleeping, and the family only had a brief opportunity to check on her condition. On November 11th, Keller and his son visited to see how their mother was doing.
“She looked very comatose, struggling to sit up. They were attempting to feed her, but her head hung low and appeared sunken,” he recalled. It was then they learned that the doctor would not be available to see her until Monday, November 14th—five days after her falls.
“My sister and I agreed that we needed to take her to the hospital. When she approached the front desk to inform staff of their decision, the response was, ‘Why?’”
Upon arriving at the hospital, the medical team confirmed that her condition was far from stable and revealed the fractures in her C1 and C2. The family’s fear was realized, emphasizing the urgent need for proper care and oversight.
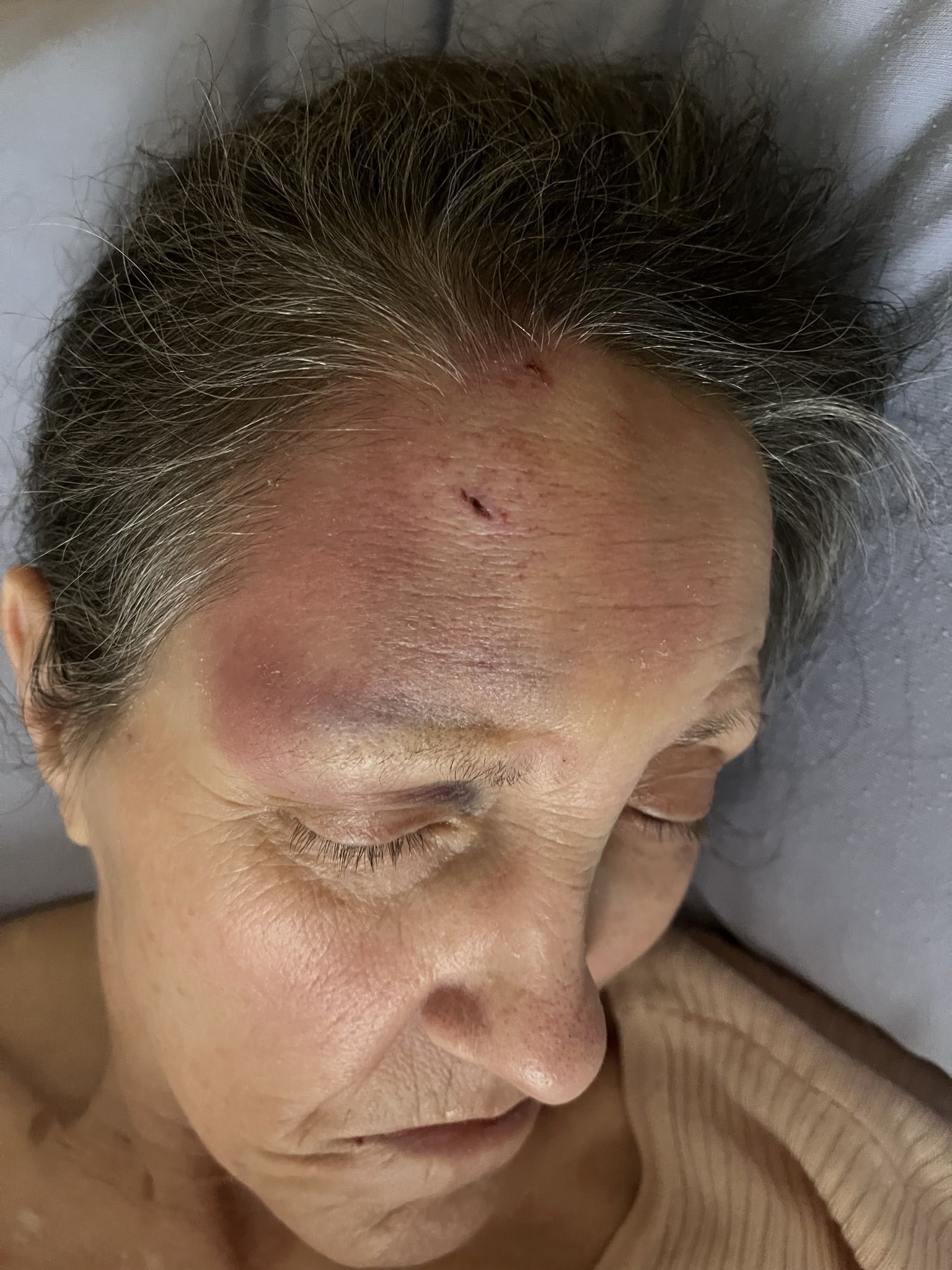
“She was clearly suffering in pain throughout this entire ordeal,” Keller said. “It’s baffling how no one recognized the severity of her condition and thought she didn’t need immediate medical attention.”
“Her health continued to deteriorate rapidly. The combination of her injuries, the unrelenting pain, and being confined to bed was too much for her to bear,” Garnot lamented. “Ultimately, she couldn’t recover from it.”
Tragically, Kelly Ashton passed away at the UNHBC hospital in Prince George on December 1st, 2022, at the age of 62. The family provided a death certificate to My PG Now; however, no documentation clarified the official cause of her death, leaving them with lingering questions.
Notably, the first words in Simon Fraser Lodge’s investigation summary state:
“On November 13, 2022, the General Manager received an email from Santaya (Garnot) requesting to halt all payments as the resident will not be returning to care…”
“…Resident was transferred to the hospital, with unclear reasons provided.”
While this tragic episode marked the most severe incident, it was not the first time the family raised concerns about care standards at Simon Fraser Lodge. Previous issues included inadequate dental care; Kelly returned from two dental appointments on November 10, 2021, and February 26, 2022, with documentation indicating severe neglect of her oral health, leading to gingivitis and inflammation.
A letter from Dr. von den Steinen, addressed to Simon Fraser Lodge on February 26, 2022, expressed deep concern over Kelly’s dental care: “We were disheartened and very disappointed to see, yet again, the severe dental neglect in Ms. Ashton’s mouth. The amount of plaque, bacteria, and food debris on her teeth and denture was disgusting and very neglectful. The buildup of bacteria and food that has accumulated on her teeth and denture is from days, if not weeks, of inadequate oral hygiene practices.”
“This kind of treatment is deplorable and shameful.”
“Kelly indicated that she was in pain, and her tissues were inflamed, irritated, and showing signs of early infection. Ms. Ashton does not possess the cognitive ability to brush her teeth, clean her denture, or perform adequate oral care independently. She has always been a very cooperative patient and has not shown any signs of resistance to treatment in our office. We don’t anticipate any difficulties with having someone assist her with her oral hygiene,” the letter continued.
Despite the clear directives and concerns raised, the family reported that there was no noticeable improvement in Kelly’s oral care after these communications.
In light of these troubling experiences, Garnot and Keller are currently exploring all legal avenues to address the situation. “We are determined to speak out,” Garnot stated firmly. “If the Lodge had approached these issues differently, acknowledging their failures and expressing genuine remorse, we might have been able to take a different path. Unfortunately, it feels as though they have ignored our concerns from the very beginning.”
“When we went to collect my mother’s belongings, they offered no words of comfort or support,” Keller recalled. “We shared a brief synopsis of what transpired, and their response was simply, ‘We’re sorry that happened.’ It lacked any sincerity or acknowledgment of the trauma we endured.”
Michele Thomson, the Vice President of Operations for Buron, the parent company of Simon Fraser Lodge, also spoke with My PG Now. Due to confidentiality laws, she could not provide specific details regarding the incidents and directed many questions back to the health records and reports shared with the family.
“We are aware of the complaint and are in communication with the family,” she stated. “These complaints are taken very seriously, and we have reported them to the appropriate regulatory bodies, authorities, and the patient quality review office.”
“It’s unfortunate that the family feels we have been apathetic or that we do not care. I assure you that we do. This outcome is not what we wanted or hoped for, and we regret that the family feels we did not respond in a way that validated their concerns.”
Travis White, the General Manager of Simon Fraser Lodge, replied to our request for an interview via email: “Thank you for reaching out. I understand you have already spoken with my VP Operations, Michele Thomson, whom I have copied on this correspondence. I do not have any further comments to add to her statement at this time.”
“It became an overwhelming series of events, leading us to consider moving her,” Garnot explained. “In hindsight, we wish we had pursued switching care homes.” Keller echoed her sentiment, mentioning discussions with Ashton’s physicians about the possibility of relocation.
“The process of switching care homes is incredibly challenging. Given my mother’s condition, she would have been placed at the bottom of the waiting list, prolonging the transition. Additionally, we were informed by her care team that relocating her at this stage would not be beneficial to her health,” Keller explained.
Both siblings acknowledged their inability to care for their mother themselves. “The reality is that switching care homes is next to impossible, and when lodging complaints, the health authority insists on working with the current facility. This approach ultimately contributed to our mother’s premature passing,” Keller lamented.
“Just six weeks after these discussions, Ashton suffered the falls that changed everything,” Garnot added. “There must be change in the system.” Keller concluded with a poignant reminder, “Deciding to place a loved one in care is one of the hardest decisions you can ever make. We need to set higher standards for care. A simple apology is insufficient.”
“There are many residents without family members to advocate for them, and we would never want another family to endure this kind of suffering,” Garnot said. According to Simon Fraser Lodge’s website, they accommodate up to 130 senior residents, specializing in dementia care.



